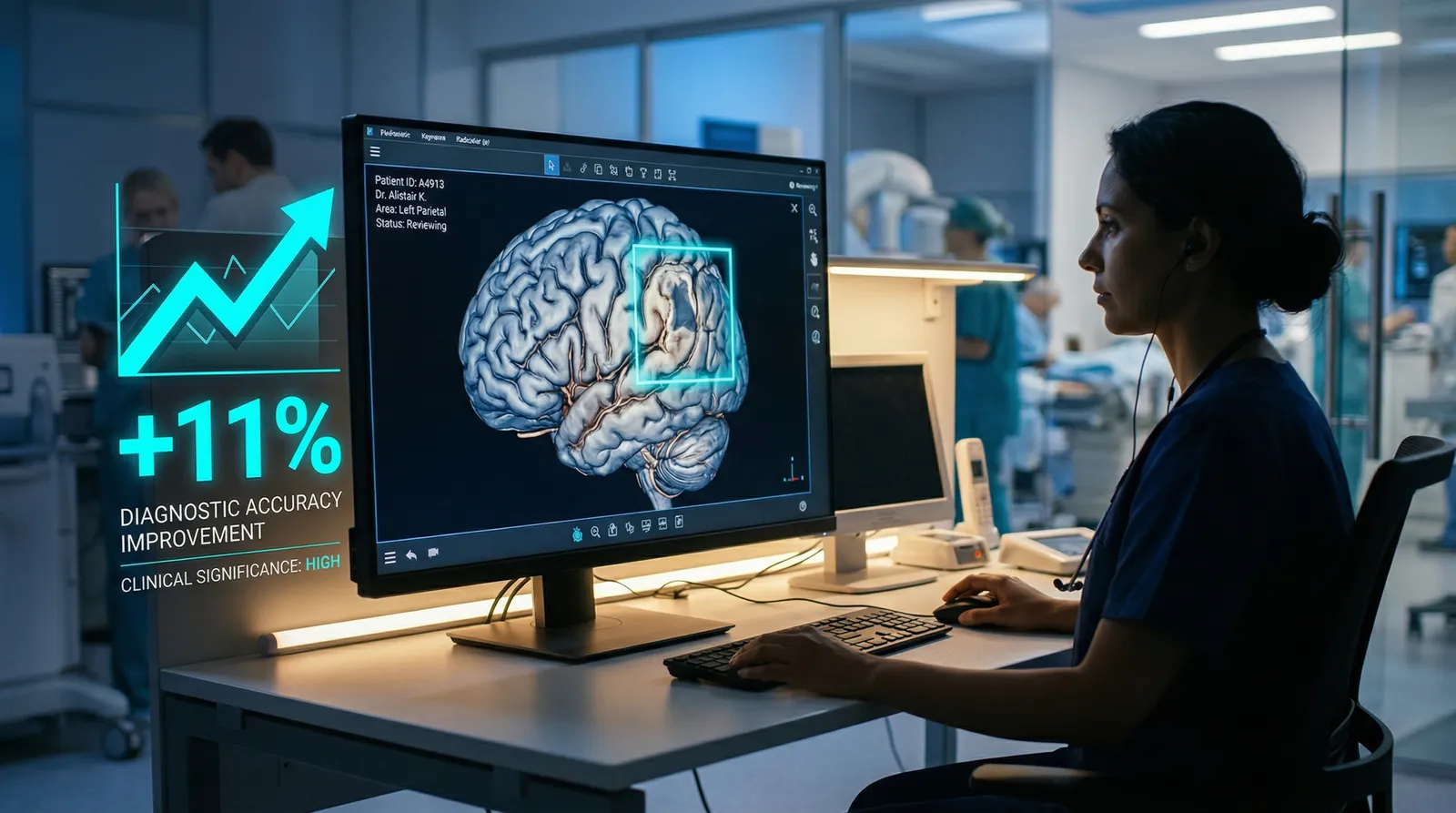
What specifically changed in MedGemma 1.5—and why does it matter clinically?
MedGemma 1.5 brought roughly a 14-percentage-point accuracy gain in MRI disease-finding classification, new support for 3D CT and MRI volumes, anatomical localization and longitudinal imaging.
Google's medical imaging model, MedGemma, moved from version 1.0 to 1.5 on January 12, 2026, with three major upgrades. The headline change: MRI disease-finding classification accuracy improved by roughly 14 percentage points over the prior version—from about 51% to 65%—with similar gains on certain CT and longitudinal imaging tasks. These gains are based on internal benchmarks across multiple disease categories in MRI and CT, not a single monolithic 3D MRI metric. But the real clinical improvements are the new capabilities the model now supports.
First, the model can now reason across three-dimensional medical scans, not just individual 2D slices. When a radiologist reviews an MRI, they're looking at a stack of thin images—think of a CT scan as a sequence of X-ray cross-sections. MedGemma 1.5 processes this entire 3D volume as one coherent image, spotting abnormalities that only become obvious when you look at how they span across multiple slices and planes.
Second, the model now outputs anatomical bounding boxes—it doesn't just say "abnormality detected," it shows you exactly where in the scan to look. A radiologist used to have to hunt through a 300-slice MRI to find what the AI flagged. Now the AI points to it with pixel-level precision.
Third, MedGemma 1.5 understands multi-timepoint imaging across modalities—MRI, CT and chest X-ray—tracking sets of scans taken weeks or months apart. This is clinically essential for oncology patients tracking tumor shrinkage during chemotherapy, or heart failure patients monitoring how their left ventricle is remodeling, or patients with chronic inflammation watching disease progression. The model can now quantify change across time, not just snapshot analysis.
Compact and deployable: why smaller wins in clinical AI
Many frontier AI models now range from tens to hundreds of billions of parameters. MedGemma 1.5 at 4B runs on commodity hardware, enabling deployment in rural hospitals and clinics worldwide.
Running a frontier medical AI model requires GPU infrastructure most hospitals can't afford or persistent cloud connectivity most rural facilities don't have. MedGemma 1.5's 4B parameters work on a single NVIDIA A100. For underserved medical centers and healthcare systems in emerging markets, that's the difference between having access to AI-assisted diagnosis and not having it.
This represents a deliberate shift in how the medical AI field is thinking about model design. Specialized, compact models consistently outperform large generalists on narrow, high-stakes domains. A small model built for radiology beats a giant multimodal model built for everything. This challenges the scaling narrative that dominated AI for the last five years.
The 14-percentage-point accuracy gain also highlights that improvements aren't coming from simply making models bigger anymore. They're coming from better datasets, smarter architectures and tuning for specific clinical tasks. MedGemma 1.5's training incorporated sequential medical imaging data—learning not just from single snapshots but from longitudinal patient records. That architectural change generated most of the accuracy jump.
Strong benchmarks, real hallucination risk
MRI disease-finding classification improved from about 51% to 65%, but hallucination risk remains: false positives, false negatives and overconfidence in ambiguous cases require radiologist oversight every time.
A 51% to 65% accuracy gain sounds like a solved problem. It isn't. The jump tells you the model improved—it doesn't tell you what happens in the scans it still reads wrong. On CT and 2D imaging tasks the gains are more modest. And accuracy numbers alone don't tell you whether the model is clinically useful; for that you need to know what kinds of mistakes it makes and in which situations it fails.
Related research published in April 2026 called RETINA-SAFE benchmarks hallucinations specifically in medical imaging AI. Hallucinations in radiology mean two things: false positives (reporting abnormalities that aren't there) and false negatives (missing real abnormalities). The research found that medical imaging models—including Gemma-based models—make these mistakes more often in ambiguous cases. When a scan shows something borderline or unusual, the model can overcommit to a diagnosis it's not sure about.
This is the critical guardrail: no radiologist should use MedGemma 1.5 (or any AI diagnostic tool) as the final decision-maker. The model is a second reader. A radiologist reviews every output, confirms the diagnosis, and takes responsibility for the clinical decision. That workflow is slower than fully automated diagnosis, but it's how medical AI is actually deployed in practice.
| Imaging Modality | MedGemma 1.5 Primary Use | Accuracy Range (Typical) | Key Limitation |
|---|---|---|---|
| 3D MRI | Tissue classification, volumetric lesion detection | ~60–65% (disease-finding) | Hallucination on edge cases |
| Sequential MRI (multi-timepoint) | Disease progression tracking, longitudinal analysis | ~60–65% (disease-finding) | Requires radiologist confirmation for treatment decisions |
| Anatomical localization | Bounding box placement, region-of-interest marking | Qualitative benefit; not pure per-pixel accuracy | Works best on major organs, less reliable on tiny structures |
| Comparative imaging | Change quantification, size/density measurements | Qualitative benefit to change detection; not pure per-pixel accuracy | False negatives on subtle changes; requires serial imaging protocols |
How can hospitals and clinics actually deploy MedGemma 1.5?
Google released MedGemma 1.5 with open weights on Hugging Face in January 2026, letting hospitals run the model locally or on private infrastructure without cloud dependency.
Google released MedGemma 1.5 with open weights available on Hugging Face shortly after the January 2026 announcement, so hospitals and developers can run the model locally or on private infrastructure. Radiology departments can integrate it into PACS workflows for automated screening and radiologist review, either on-premise or in private-cloud environments, reducing reliance on proprietary cloud APIs.
For radiology departments and diagnostic imaging centers, this means integration points. A hospital's PACS system receives DICOM-formatted imaging files—the standard format used by every major MRI and CT scanner—and routes them to MedGemma 1.5 for automatic screening. The model flags regions of interest and outputs bounding boxes. A radiologist reviews, confirms or overrides and signs off. The entire workflow is auditable and integrated locally.
For international development and underserved healthcare, the compact size is transformative. A rural clinic in sub-Saharan Africa or South Asia can run MedGemma 1.5 on modest hardware. Medical training can be scaled up without requiring infrastructure parity with US hospitals.
What MedGemma 1.5 signals about medical AI's direction
One data point doesn't make a trend, but MedGemma 1.5 fits a pattern emerging across high-stakes AI domains: specialized, compact models outperforming large generalists on narrow tasks. The medical AI field is shifting from "how big can we make it?" to "how small can we make it while clearing FDA review?" That's a real inversion of where the field was two years ago.
Regulatory pressure and clinical adoption timelines are replacing raw benchmark scores as the limiting factors. A model doesn't need top performance on every dataset—it needs to run on hardware hospitals already own, integrate with PACS and DICOM workflows and hold up under clinical audit requirements. MedGemma 1.5 clears all three bars. The 14-point accuracy gain was almost secondary to the deployability story.
What to watch: whether this compact, audit-ready approach gets adopted at scale by hospital systems, or stays a developer proof-of-concept. FDA clearance timelines will determine that—not benchmark leaderboards.
Sources
- MedGemma 1.5 Model Card and Technical Notes — Google Health AI Developer Foundations
- Next-Generation Medical Image Interpretation with MedGemma 1.5 — Google Research Blog
- MedGemma 1.5 4B Instruct — Hugging Face Model Card (google/medgemma-1.5-4b-it)
- Medical AI Imaging Market Report, Grand View Research (2026)
Related Articles on Nexairi
The Nexairi Technology Desk covers emerging technologies, artificial intelligence, data infrastructure, policy, and the forces reshaping how we work and build. Our reporting combines primary research with human editorial oversight.
More from this desk